Insights
Case Study | Regional Blues Plan
A HealthHelp client was experiencing provider dissatisfaction with their UM process along with a high denial rate. Savings was coming from denials and not care focused on improved outcomes. We worked in partnership to implement our collaborative and proactive provider outreach model along with our clinically superior tech.
Denials reduced by 50% | Savings and Provider Satisfaction Increase
Commercial Program
(Cardiology, MKS, Sleep, Surgical)
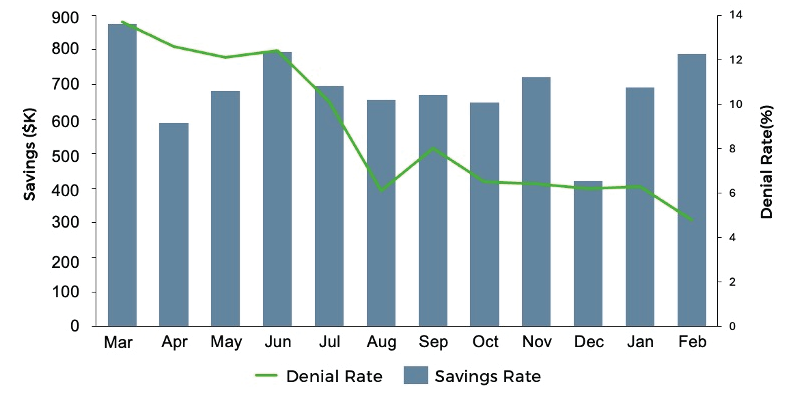
Initial Challenge
- High prior-auth denial rate
- Provider dissatisfaction
- Savings through denial
HealthHelp Solution
- Proactive outreach to providers
- Supported providers with clinical education by top-tier specialist
- Providers chose modification or withdrawl, reducing denials
Outcomes
- Net direct savings ROI: 4.9
- Annualized savings rate of $8M
- Reduced denials/abrasion
- Provider NPS: 60

About WNS-HealthHelp
HealthHelp, a unit within WNS, is a trusted healthcare technology platform for health plans’ clinical programs for over 25 years. Our unified suite of Advanced AI powered technology platform-based solutions simplifies medical complexity and workforce challenges, and enhances provider relations and member journeys (i.e., customer experiences). Our uniquely designed UM and clinical solutions were developed to fit into health plans’ existing clinical programs to advance outcomes and success. We work in partnership to understand health plan commercial and Medicare clinical programs, and determine where our solutions can advance outcomes and lower cost. There is no one size fits all, and we know how to expediently deliver the best tailored solution for a specific health plan’s needs.
Related Articles
Navigating Recent CMS Mandates with Intelligent Technology and Smarter Utilization Management
WNS-HealthHelp Executive outline how regulatory expectations are evolving beyond administrative compliance and how to prepare for success in the new landscape.
Orchestrating Intelligent Prior Authorization for Collaborative Care
WNS-HealthHelp explores how health plans combining are transforming the UM landscape with AI, HI, and Automation.
Elevating Utilization Management: A Digitally Powered Model for Cost, Compliance, and Care
WNS-HealthHelp explores how health plans combining are transforming the UM landscape with AI, HI, and Automation.



